Updated 8/31/22
Read time: 7 minutes
If you’re frustrated that your blood sugar, or A1C, hasn’t gone down despite your best efforts to eat in a way that aligns with your health goals and incorporate more physical activity into your daily routine, know that there's more to your numbers than meets the eye.
Think about this:
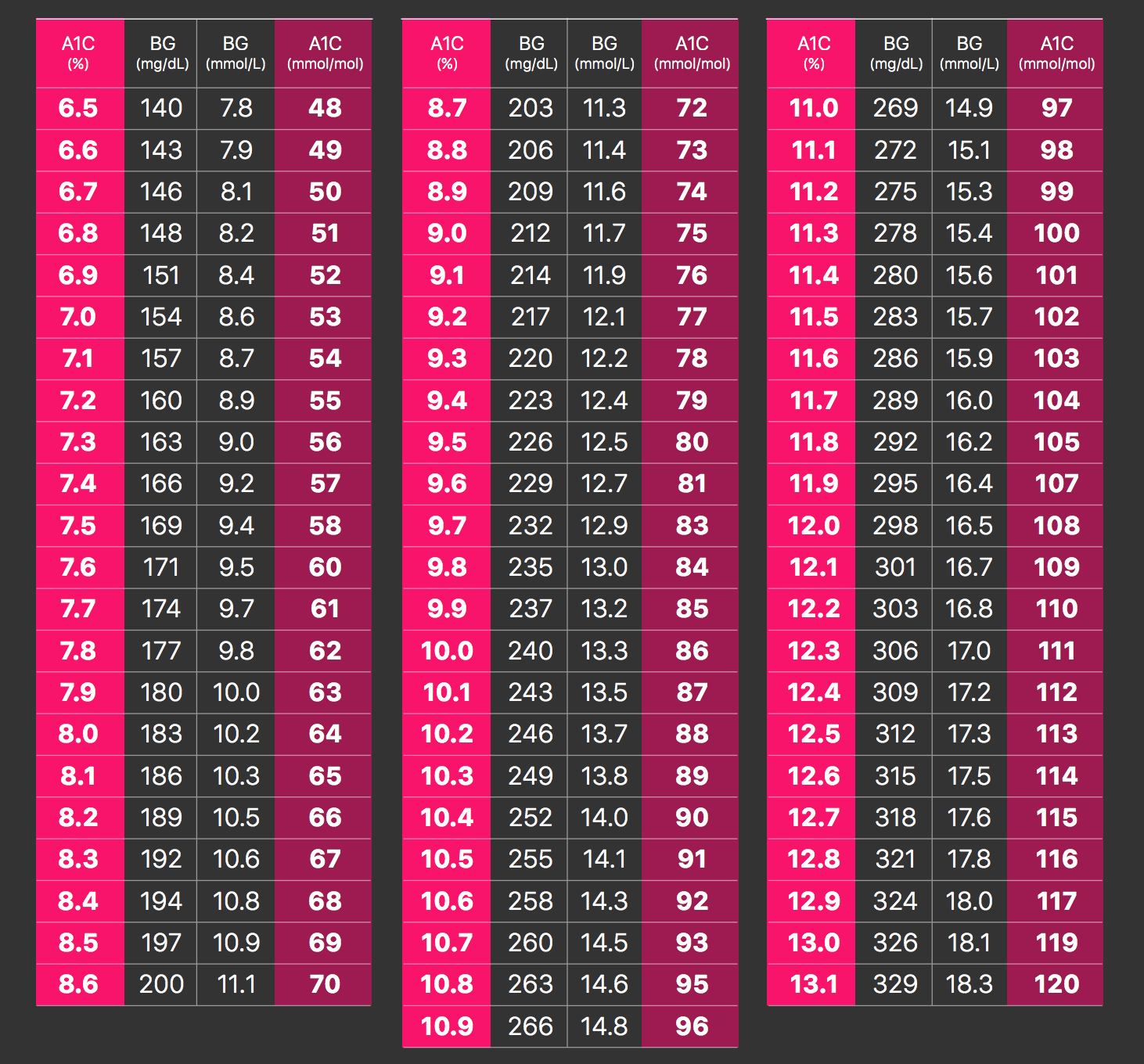
Your A1C is the culmination of your blood sugar levels over the course of the prior two to three months. The A1C can be translated to an estimated average glucose (eAG). For example, an A1C of 8.0% infers an eAG of 183 mg/dL. (The chart below shows the conversion.)
An average blood sugar of 183 mg/dL means that blood sugar is higher than 183 mg/dL some of the time and lower than 183 mg/dL some of the time.
Meanwhile, an A1C of 7.0% translates to an estimated average glucose of 154 mg/dL. That means that aiming for a mere 30 mg/dL lower average blood sugar could translate to a 1% difference in A1C!
RELATED CONTENT
The Ultimate Guide to A1C
High Blood Sugar vs. Higher-Than-Average Blood Sugar
The trick, in this scenario, is to adjust the way you're thinking of "high" blood sugar. Many of us know that 300 mg/dL is "high." But, if you're looking to get an 8.0% A1C down to 7.0%, it could be helpful to view 183 mg/dL as "high" as well.
It might sound easy, but when you put it into practice, it can be a little tricky.
If your goal is to reduce your A1C, here are some helpful tips to change your mindset and reach your goals.
Step 1: Get to the Root of the Problem
You can’t fix something until you know (and understand) the root cause of the problem.
Ask yourself: "What have I been considering a high blood sugar?" Perhaps you need a full week of observing and reflecting on your blood sugar patterns and trends.
By the end of the week, you could learn something new such as that your highest readings are often after lunch or that you spend the majority of your workday around 200 mg/dL. If you're used to these patterns as being "your normal," you may not have considered changing your habits to reduce these highs.
RELATED CONTENT
What Causes High Blood Sugar and How to Prevent It
Step 2: Set a New Standard of Success (a.k.a. Identify a New High)
Decide on your new standard of "high blood sugar." Using your goal A1C may be a good starting place.
For instance, if your goal is an A1C of less than 7%, that means aiming for an average blood sugar of less than 154 mg/dL.
In this example, you might decide that you’ll take action to correct any patterns of blood sugar over 154 mg/dL by modifying your meals or movement habits or talking to your doctor about adjusting your insulin dosing.
When determining your ideal blood sugar range, check in with yourself (and your doctor) to make sure your target is realistic and safe. Trading high blood sugar levels for low blood sugar levels (under 70 mg/dL) is dangerous and not beneficial to your health.
Remember, the focus is on progress, not perfection. Whatever your new goal is, write it down where you'll see it and embrace your new range as your new goal.
Step 3: Tighten Up Fasting Blood Sugar
Take a look at your fasting blood sugar. If you’ve been seeing 160 mg/dL on your meter or CGM in the mornings and don't do anything about it, that could contribute to your A1C frustration.
It could mean that you’ve spent all night with a blood sugar well above your target range or that you're experiencing the Dawn Phenomenon. of your target A1C. Getting to the bottom of elevated fasting blood sugar may help explain why your A1C is higher than your goal, even if you've been staying closer to your goal range during the day.
Remember, the eight hours you are sleeping each night make up a third of your A1C result! Keep an eye on your overnight blood sugar and work with your One Drop clinical health coach and doctor adjust your habits and medication doses accordingly.
RELATED CONTENT
What Exactly is a Health Coach?
Step 4: Pinpoint Other Blood Sugar Trouble Spots
Remember that week of observing and reflecting on your blood sugars suggested in Step One? Go through your observations carefully and take a look at each individual pattern.
If blood sugar is high after a particular meal, consider reducing your carbs, adding movement around that time, or questioning your mealtime insulin dosing.
If you notice that a pattern of stressful events causes highs, consider when you could incorporate stress management techniques into your day.
If you usually exercise with your blood sugar around 200 mg/dL because you’re terrified of going low, learning how to exercise with in-range blood sugar can help to get you closer to your A1C goal. Managing blood sugar while exercising isn't always easy, but it can be done. Consider checking out The Athlete’s Guide to Diabetes by Sheri Colberg, PhD for more information on managing blood sugar during exercise or Bright Spots & Landmines by Adam Brown for in-depth guidance on overall pattern management
In the end, it’s all about learning, studying, and adjusting. When you’re ready to focus on reducing your A1C, make sure that your idea of a “normal” blood sugar vs. a high blood sugar lines up realistically with your goals.
This article has been clinically reviewed by Alexa Stelzer, RDN, LD, CDCES, clinical health coach at One Drop.